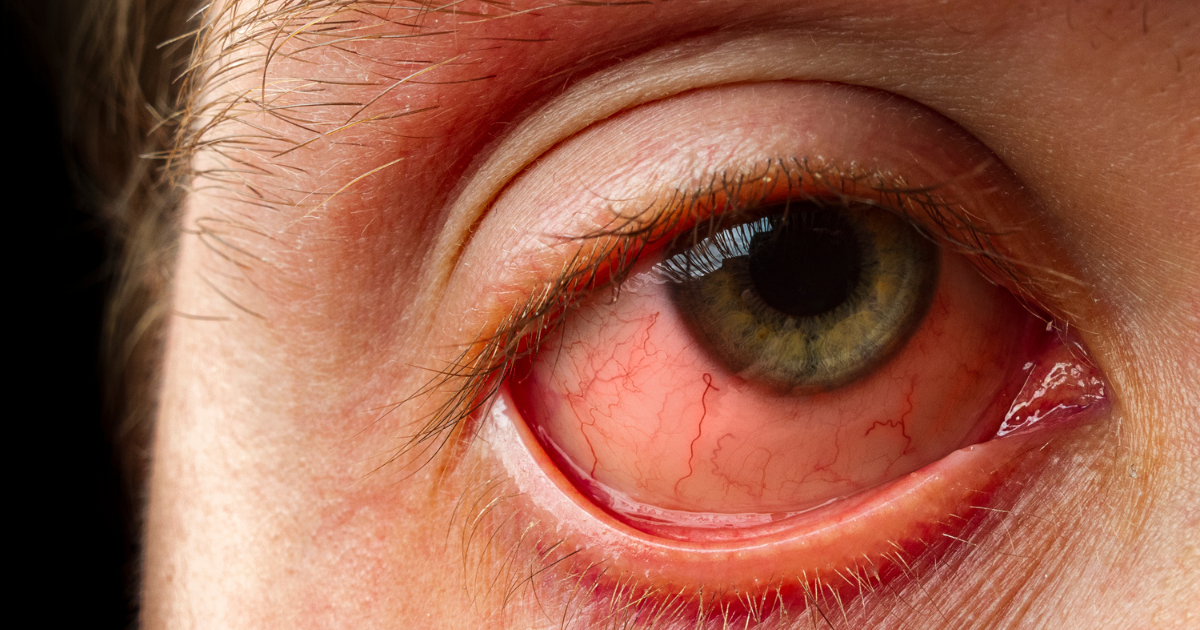
Winter can be tough for people living with Systemic Lupus Erythematosus (SLE) — commonly known as Lupus. The drop in temperature, dry air, and limited sunlight often make joint pain, skin problems, and fatigue worse.
If you have Lupus, you might notice that your body feels stiffer, your skin becomes dry or rash-prone, and your energy levels dip during cold months.
This happens because winter brings multiple triggers — weaker immunity, reduced vitamin D, and poor blood circulation.
But with the right care, you can enjoy the season while keeping your symptoms in control.
Let’s understand how to take care of your skin, joints, and immune system during winter.
1. Why Winter Makes Lupus Symptoms Worse
Lupus is an autoimmune disease, where your immune system mistakenly attacks healthy tissues.
Cold weather adds extra challenges:
- Low sunlight → causes Vitamin D deficiency, which affects bones and immunity.
- Cold air → tightens blood vessels, reducing blood flow to joints and muscles.
- Dry air → damages the skin barrier and worsens rashes or discoid lupus.
- Infections → are more common in winter, which can trigger Lupus flares.
Understanding these effects helps you plan your daily routine to minimize discomfort.
2. Skin Care Tips for Lupus Patients in Winter
People with Lupus often have sensitive and photosensitive skin, which means both sun and cold can cause rashes or irritation.
Follow these skin-friendly steps:
a) Keep Skin Moisturized
Use fragrance-free, hypoallergenic moisturizers at least twice daily.
Apply immediately after bathing to lock in moisture.
b) Use Sunscreen Daily
Even in winter, UV rays can trigger skin flares.
Choose a broad-spectrum SPF 30 or higher sunscreen, and apply it on your face, neck, and hands.
c) Protect from Cold Wind
Wear soft cotton or wool-blend scarves and gloves to protect skin from dryness and windburn.
d) Avoid Hot Water Baths
Very hot water strips natural oils from the skin.
Instead, use lukewarm water for bathing and apply moisturizer right after.
e) Choose Mild Products
Avoid harsh soaps and alcohol-based lotions that can worsen sensitivity.
3. Joint and Muscle Care
Joint stiffness and pain are common in Lupus, and cold weather can make them worse.
To ease discomfort, follow these practical steps:
a) Stay Warm
Keep your body temperature steady. Wear layered clothing and cover joints when going outdoors.
b) Gentle Movement
Avoid sitting in one position for too long.
Light stretching, yoga, or walking can keep your joints flexible.
c) Heat Therapy
Use heating pads or warm compresses to relax muscles and relieve stiffness.
d) Continue Medications
Never stop prescribed medications like Hydroxychloroquine or Immunosuppressants during winter — even if you feel better. They help prevent flare-ups.
e) Maintain Good Posture
Sit upright, use supportive chairs, and avoid bending for long periods to protect your spine and hips.
4. Boosting Immunity During Winter
Lupus and its medications can weaken the immune system. During winter, you need extra protection against colds, flu, and infections.
Here’s how:
a) Eat an Immunity-Boosting Diet
Include Vitamin C–rich fruits (oranges, amla), green vegetables, garlic, turmeric, and ginger. Omega-3 fatty acids from fish, flaxseed, or walnuts help reduce inflammation.
b) Check Your Vitamin D Levels
Sunlight exposure is limited in winter. Ask your doctor about Vitamin D supplements if needed.
c) Prioritize Sleep
Lack of sleep triggers inflammation. Try to get 7–8 hours of restful sleep daily.
d) Manage Stress
Meditation, breathing exercises, or mild yoga can reduce stress hormones that worsen lupus symptoms.
e) Get Vaccinated
Annual flu shots or other vaccines (as advised by your doctor) help reduce infection risk.
5. Lifestyle Habits for Winter Wellness
Lupus management is not only about medication — daily habits matter too.
- Stay hydrated — Drink enough water; dehydration worsens fatigue.
- Avoid smoking — It damages blood vessels and worsens lupus flares.
- Exercise indoors — If it’s too cold outside, practice yoga or light stretching indoors.
- Take breaks — Don’t overexert; fatigue is common in lupus.
- Maintain regular doctor visits — Routine monitoring helps prevent complications.
6. Emotional Health Matters
Winter blues or seasonal depression can make lupus symptoms feel heavier.
Stay connected with friends, maintain a routine, and express how you feel.
Emotional well-being plays a big role in physical health.
If you feel persistently low, don’t hesitate to talk to your doctor or counselor.
Conclusion
Lupus may be unpredictable, but you can control how it affects you — especially in winter. By following simple skin care, joint protection, and immunity-boosting tips, you can minimize flare-ups and enjoy a healthier season.
Remember:
- Keep your body warm.
- Protect your skin.
- Eat well and rest enough.
- And most importantly — stay positive and consistent with treatment.
With mindful care, winter doesn’t have to be a challenge — it can be a season of comfort and control.
FAQ (Frequently Asked Questions)
1. Why do lupus symptoms get worse in winter?
Cold temperatures reduce blood flow and increase inflammation, leading to joint stiffness and skin dryness.
2. Can sunlight in winter help lupus patients?
Limited sun exposure may help Vitamin D levels, but too much can worsen photosensitive rashes. Always use sunscreen.
3. What foods help reduce lupus flare-ups in winter?
Include omega-3-rich foods, turmeric, green vegetables, and vitamin-rich fruits. Avoid processed and fried foods.
4. How can lupus patients prevent winter infections?
Stay vaccinated, avoid crowded places, wash hands regularly, and maintain good sleep and nutrition.
5. Can hot showers worsen lupus skin symptoms?
Yes. Hot water removes skin oils, causing dryness and irritation. Use lukewarm water instead.