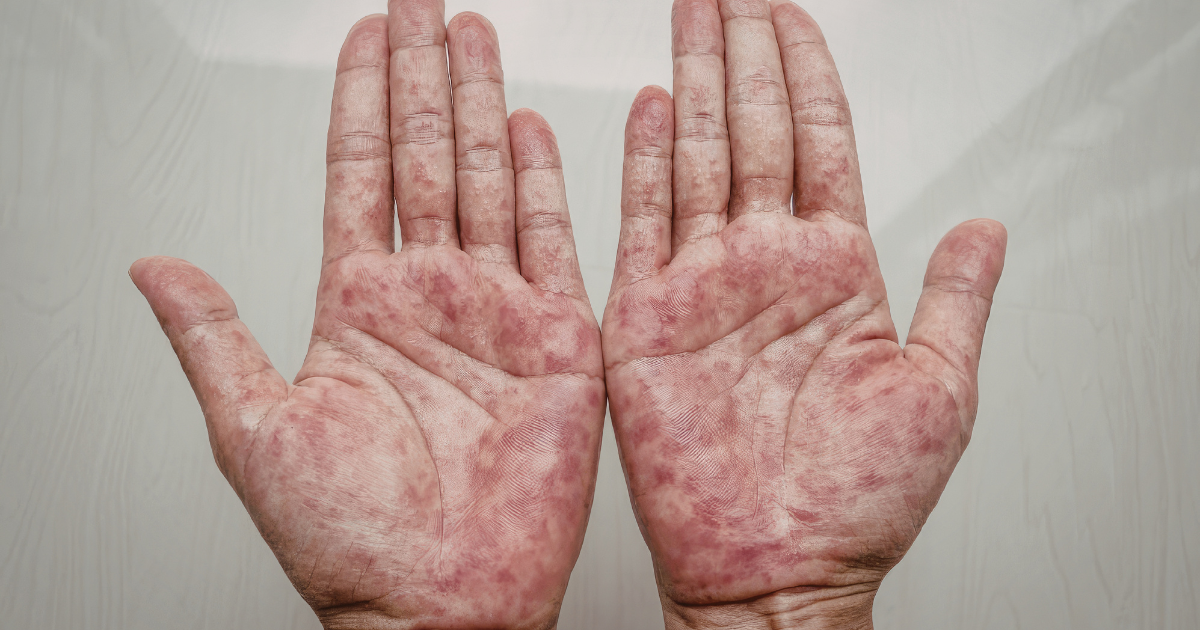
Lupus, or Systemic Lupus Erythematosus (SLE), is a chronic autoimmune condition where the immune system mistakenly attacks the body’s own tissues. It can affect the skin, joints, kidneys, heart, lungs, and brain, leading to a wide range of symptoms. While traditional treatments include corticosteroids, antimalarial drugs, and immunosuppressants, these options can come with long-term side effects. In recent years, immunotherapy has emerged as a promising approach in the management of lupus.
What Is Immunotherapy?
Immunotherapy is a form of treatment that modifies or regulates the immune system’s response. Unlike general immunosuppressants that suppress the immune system entirely, immunotherapy aims to target specific components of the immune system that are malfunctioning. This precision makes immunotherapy a game-changer in treating autoimmune diseases like lupus.
How Immunotherapy Works in Lupus
In lupus, the immune system produces autoantibodies that attack healthy tissues. Immunotherapy works by:
- Blocking specific immune pathways involved in the production of these harmful autoantibodies.
- Inhibiting B-cells (the white blood cells that create autoantibodies), which play a central role in lupus inflammation.
- Modifying cytokines, which are signaling proteins that drive inflammation and tissue damage.
By selectively altering these immune responses, immunotherapy can reduce lupus flares and disease activity while minimizing damage to the rest of the immune system.
Key Immunotherapy Drugs for Lupus
Several immunotherapy agents have been studied and are now in use or in clinical trials for lupus. Some notable ones include:
1. Belimumab (Benlysta)
Belimumab is the first biologic approved specifically for lupus. It targets a protein called BAFF (B-cell activating factor), which helps B-cells survive and multiply. By reducing BAFF, Belimumab limits the activity of autoantibody-producing B-cells, thereby reducing disease severity.
2. Rituximab
Originally used for certain cancers and rheumatoid arthritis, Rituximab targets CD20-positive B-cells. Though not formally approved for lupus, it has shown promise in patients with severe lupus, especially those resistant to conventional treatments.
3. Anifrolumab (Saphnelo)
A newer FDA-approved therapy, Anifrolumab targets the type I interferon receptor, a key pathway involved in lupus inflammation. It has shown to reduce disease activity and the need for steroids in many lupus patients.
Benefits of Immunotherapy in Lupus
- Targeted treatment: Acts on specific immune functions rather than suppressing the entire system.
- Reduced flares: Many patients experience fewer lupus flares.
- Lower steroid dependency: Reduces the need for high-dose steroids, which have serious side effects over time.
- Better quality of life: Improved symptom control means better physical and mental well-being.
Risks and Considerations
Despite its promise, immunotherapy is not without challenges:
- Infections: Altering the immune system can make patients more prone to infections.
- High cost: Biologic drugs are expensive and may not be accessible to all.
- Variable response: Not all patients respond the same; genetic and disease variations influence effectiveness.
It’s crucial for patients to work closely with their rheumatologist to monitor side effects and evaluate whether immunotherapy is the right choice for them.
The Future of Immunotherapy in Lupus
Research continues to explore new immunotherapy targets, including T-cell regulation, cytokine modulation, and gene editing. Personalized medicine, where treatment is tailored to an individual’s genetic and immune profile, is likely the future of lupus care.
Final Thoughts
Immunotherapy is changing the landscape of lupus treatment by offering a more targeted and potentially safer alternative to traditional therapies. While it’s not a cure, it represents hope for many patients seeking better disease control with fewer side effects. As research progresses, immunotherapy could become a cornerstone in the long-term management of lupus.