Introduction
Behçet’s disease (BD) is a rare but potentially serious autoimmune disorder that causes blood vessel inflammation (vasculitis) throughout the body. First described by Turkish dermatologist Dr. Hulusi Behçet in 1937, the disease primarily affects the mouth, eyes, skin, joints, and sometimes vital organs like the brain, lungs, or gastrointestinal tract. Although it is uncommon worldwide, certain regions such as Turkey, the Middle East, and East Asia report higher prevalence.
Understanding Behçet’s disease is important because its symptoms often mimic other conditions, making diagnosis challenging. Without timely treatment, the disease can cause severe complications, especially vision loss and organ damage.
Causes and Risk Factors
The exact cause of Behçet’s disease is not fully known. However, research suggests it results from a combination of genetic, environmental, and immune system factors.
- Genetics: People carrying the gene HLA-B51 are at higher risk.
- Autoimmunity: In BD, the immune system mistakenly attacks the body’s own blood vessels, leading to widespread inflammation.
- Environmental Triggers: Viral or bacterial infections may trigger symptoms in genetically susceptible individuals.
- Geography & Ethnicity: More common in countries along the “Silk Road” (Turkey, Iran, China, Japan).
- Age & Gender: Typically appears between ages 20–40; men may have more severe disease, but women are also affected.
Common Symptoms
Behçet’s disease symptoms vary widely from person to person and can flare up, then subside. Key features include:
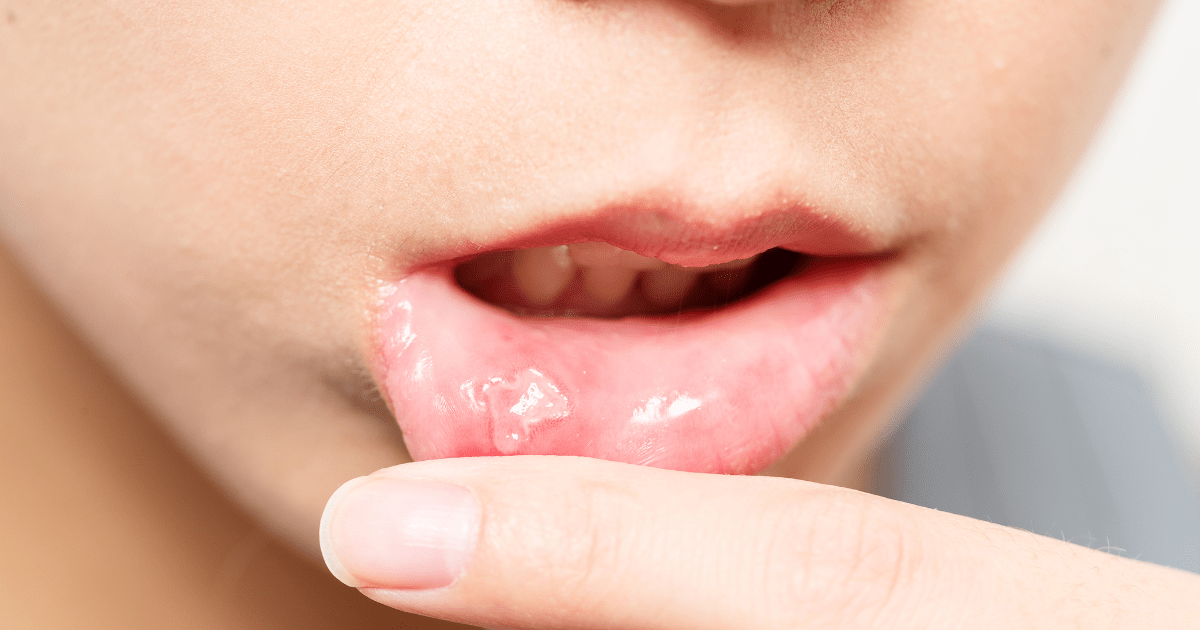
1. Oral Ulcers
- Painful, recurrent mouth sores (similar to canker sores).
- One of the most consistent and early symptoms.
2. Genital Ulcers
- Painful lesions on the genitals, often healing with scarring.
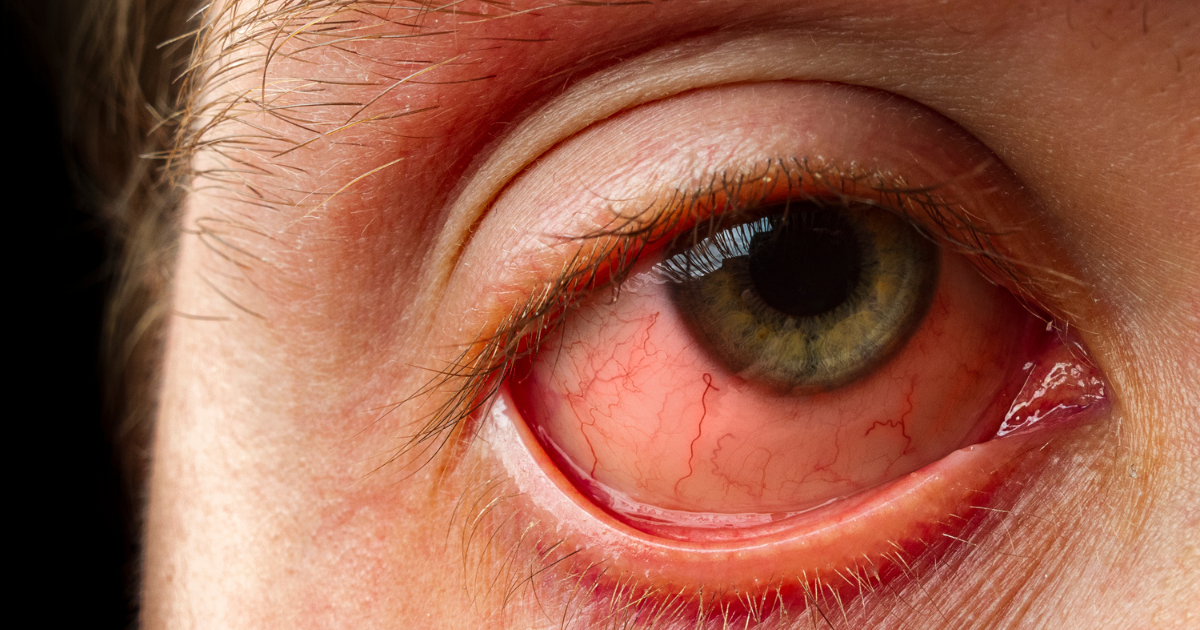
3. Eye Inflammation (Uveitis)
- Red, painful eyes, blurred vision, or light sensitivity.
- Can cause permanent blindness if untreated.
4. Skin Lesions
- Acne-like bumps, nodules, or rashes, especially on the legs.
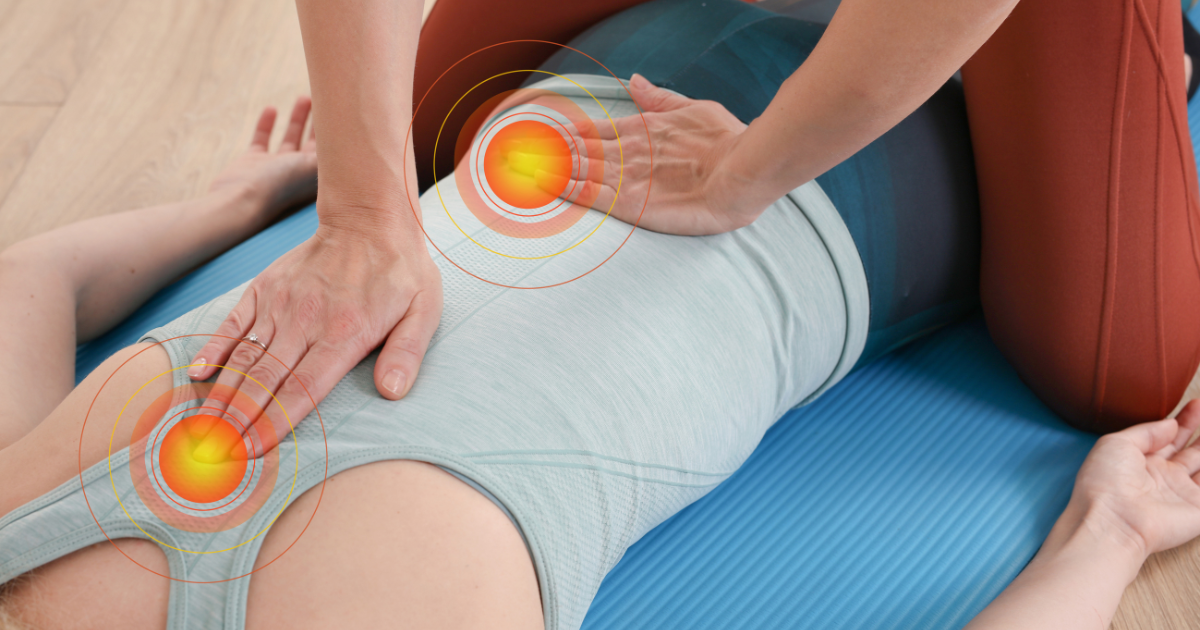
5. Joint Pain
- Arthritis-like symptoms, particularly in knees, ankles, elbows, and wrists.
6. Vascular Involvement
- Inflammation of arteries and veins leading to clots, aneurysms, or blocked vessels.
7. Neurological Involvement
- Headaches, stroke-like symptoms, memory or balance problems.
8. Gastrointestinal Problems
- Abdominal pain, diarrhea, or bleeding due to intestinal ulcers.
Diagnosis
No single test confirms Behçet’s disease. Diagnosis is clinical and often delayed due to symptom overlap with other conditions. Doctors usually rely on:
- Medical History & Physical Exam
- Criteria: Recurrent oral ulcers plus at least two of the following – genital ulcers, eye inflammation, skin lesions, or positive pathergy test (skin prick test showing abnormal immune reaction).
- Imaging & Lab Tests: MRI, blood tests, and angiography to detect organ involvement and rule out other conditions.
Complications
Behçet’s disease can be life-threatening if vital organs are affected. Possible complications include:
- Vision Loss: From repeated eye inflammation.
- Blood Clots & Aneurysms: Due to inflamed blood vessels.
- Stroke & Neurological Issues: If the brain’s blood vessels are affected.
- Organ Damage: In lungs, kidneys, or digestive tract.
Treatment Options
Although there is no cure, treatment focuses on controlling inflammation, reducing flares, and preventing complications.
1. Medications
- Topical treatments: Creams, gels, or mouth rinses for ulcers.
- Corticosteroids: To reduce inflammation during flare-ups.
- Colchicine: Effective for mouth, genital ulcers, and arthritis.
- Immunosuppressants: Azathioprine, Cyclosporine, Cyclophosphamide for severe disease.
- Biologic therapies: TNF inhibitors (e.g., Infliximab, Adalimumab) for eye and systemic involvement.
2. Lifestyle & Self-Care
- Avoid stress and infection triggers.
- Maintain good oral hygiene to reduce ulcers.
- Balanced anti-inflammatory diet (rich in omega-3 fatty acids, vegetables, whole grains).
- Regular exercise to support joint health.
- Stop smoking to reduce vascular risks.
3. Regular Monitoring
Since BD can affect multiple organs, ongoing follow-up with specialists (rheumatologist, ophthalmologist, dermatologist, neurologist) is essential.
Living with Behcet’s Disease
Managing a chronic illness can be emotionally and physically exhausting. Support groups, counseling, and patient education help individuals cope better. Early diagnosis, appropriate treatment, and consistent follow-up improve quality of life and reduce long-term complications.
Key Takeaways
- Behçet’s disease is a rare autoimmune disorder that inflames blood vessels throughout the body.
- Symptoms include oral and genital ulcers, eye inflammation, skin lesions, joint pain, and sometimes neurological or vascular involvement.
- Timely diagnosis is crucial to prevent severe complications like blindness or stroke.
- Treatments include corticosteroids, immunosuppressants, and biologic therapies.
- With proper care, patients can manage flares and lead a near-normal life.
FAQs
Q1. Is Behçet’s disease curable?
No, but it can be managed effectively with medications and lifestyle changes.
Q2. Can it affect children?
Yes, although rare, Behcet’s can occur in children and teens.
Q3. Which doctor should I consult?
A rheumatologist is the primary specialist, with referrals to eye and skin specialists if needed.
Q4. What triggers flare-ups?
Stress, infections, hormonal changes, and certain environmental factors may trigger symptoms.