What Is Juvenile Dermatomyositis?
Juvenile Dermatomyositis (JDM) is a rare autoimmune inflammatory disease that mainly affects children between 5 and 15 years of age. It causes muscle weakness and distinctive skin rashes due to inflammation of muscles and small blood vessels.
Unlike adult dermatomyositis, JDM has some unique features and requires early diagnosis to prevent long-term complications.
Common Symptoms of Juvenile Dermatomyositis
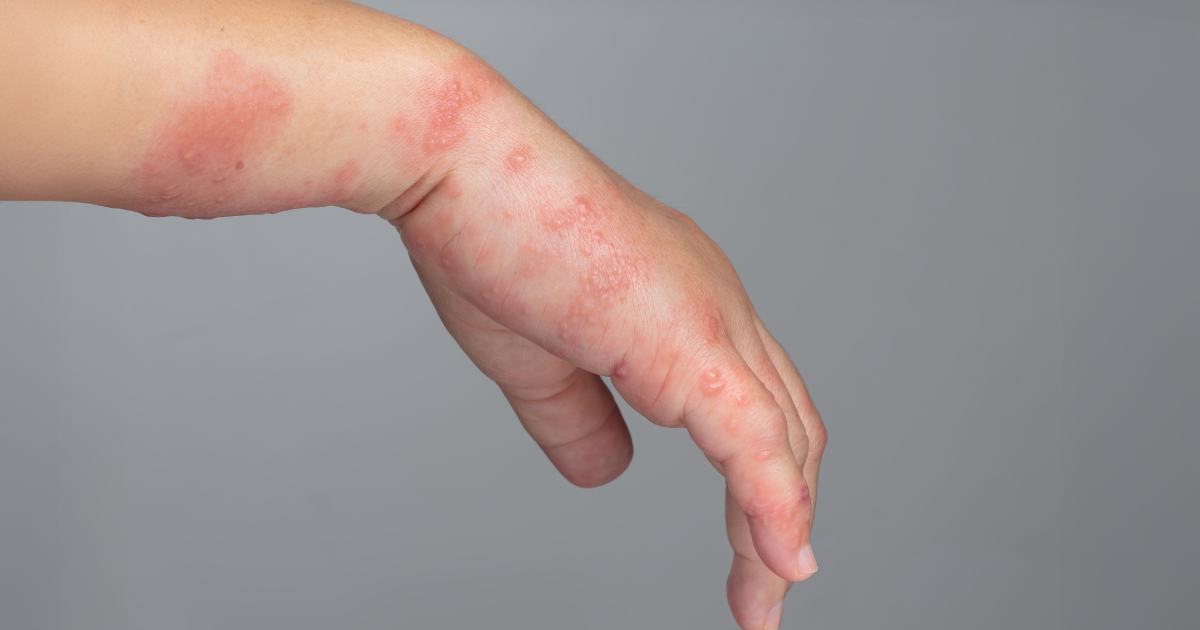
Skin Symptoms
- Purple or bluish rash around the eyes (Heliotrope rash)
- Raised reddish-purple bumps on knuckles, elbows, or knees (Gottron’s papules)
- Rash on neck, shoulders, and upper chest (Shawl sign)
- Worsening of rash after sun exposure
- Dry, scaly, or itchy skin
Muscle Symptoms
- Difficulty climbing stairs or getting up from the floor
- Trouble lifting arms or combing hair
- Muscle pain or tenderness
- Easy fatigue and reduced physical activity
- Delayed motor skills in younger children
Other Symptoms
- Low-grade fever
- Weight loss
- Difficulty swallowing
- Abdominal pain
- Calcium deposits under the skin (Calcinosis) in some children
Causes of Juvenile Dermatomyositis
The exact cause of JDM is unknown, but possible triggers include:
- Autoimmune reaction where the immune system attacks healthy tissues
- Viral or bacterial infections
- Genetic susceptibility
- Environmental factors
- Ultraviolet (UV) light exposure, which may worsen skin symptoms
How Is Juvenile Dermatomyositis Diagnosed?
Doctors may recommend a combination of tests, including:
- Blood tests (CPK, ESR, CRP, ANA, myositis-specific antibodies)
- MRI scan to detect muscle inflammation
- Electromyography (EMG)
- Skin or muscle biopsy in selected cases
Early diagnosis is essential to prevent muscle damage and complications.
Treatment Options for Juvenile Dermatomyositis
Although there is no permanent cure, Juvenile Dermatomyositis is highly treatable and manageable.
Medications
- Corticosteroids to reduce inflammation
- Immunosuppressive drugs (Methotrexate, Azathioprine)
- IVIG (Intravenous Immunoglobulin) for severe cases
- Biologic therapies if standard treatment fails
Supportive Care
- Physiotherapy to maintain muscle strength and flexibility
- Sun protection (sunscreen, protective clothing)
- Balanced diet rich in protein, calcium, and vitamin D
Regular follow-ups with a pediatric rheumatologist
Tips for Parents and Caregivers
- Do not ignore persistent muscle weakness or unusual rashes
- Ensure strict medication adherence
- Protect the child from direct sunlight
- Encourage gentle physical activity
- Attend regular medical check-ups
Frequently Asked Questions (FAQs)
Q1. Is Juvenile Dermatomyositis curable?
While there is no permanent cure, many children achieve remission with timely and proper treatment.
Q2. Is Juvenile Dermatomyositis contagious?
No, it is not an infectious or contagious disease.
Q3. Can children with JDM attend school?
Yes, most children can attend school with appropriate activity modification.
Q4. Is this a lifelong condition?
Some children recover completely, while others may need long-term monitoring.
Conclusion
Juvenile Dermatomyositis is a serious but manageable autoimmune condition. Early diagnosis, appropriate medical care, and strong family support can help children lead healthy and active lives.
If your child shows persistent muscle weakness or unusual skin rashes, consult a pediatric rheumatologist without delay.