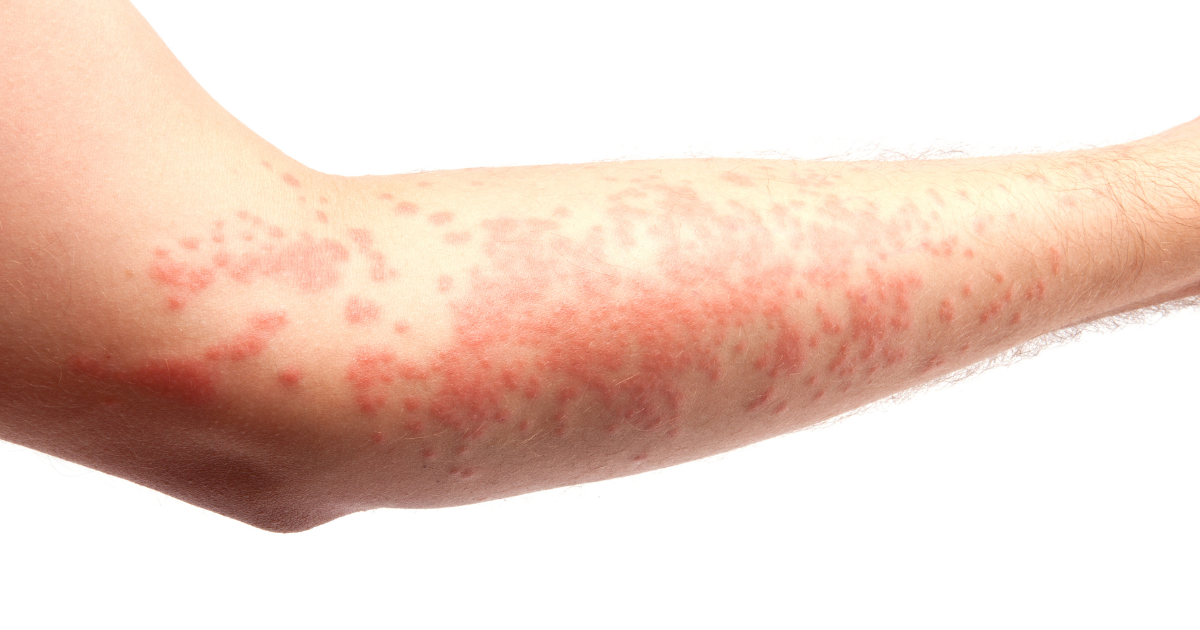
Dermatomyositis (DM) is a rare autoimmune disease that affects both skin and muscles, leading to characteristic rashes and progressive muscle weakness. Because it is uncommon and often misunderstood, many myths circulate among patients, families, and even on social media. These myths can cause confusion, fear, delayed diagnosis, or inappropriate expectations from treatment.
This detailed guide separates myths from facts, helping patients understand the condition better and manage it with confidence.
Myth 1: Dermatomyositis is Just a Skin Disease
Fact:
Dermatomyositis affects skin, muscles, lungs, joints, and sometimes internal organs.
Although skin symptoms (heliotrope rash, Gottron’s papules) are the first signs many people notice, DM is fundamentally a systemic autoimmune disorder. Most patients also develop:
- Muscle weakness
- Difficulty climbing stairs or lifting objects
- Fatigue
- Trouble swallowing (dysphagia)
- Lung involvement (Interstitial Lung Disease – ILD)
Some patients may have “amyopathic dermatomyositis,” where skin lesions appear without muscle weakness, but organs may still be at risk.
This makes proper monitoring essential.
Myth 2: Dermatomyositis Only Affects Older Adults
Fact:
DM can affect people of any age, including children.
There are two main forms:
- Adult-onset Dermatomyositis (ADM)
- Juvenile Dermatomyositis (JDM) — commonly appears between ages 5–15
Juvenile DM often presents with calcium deposits under the skin (calcinosis), while adults may have higher cancer association. Age does not protect anyone from the disease.
Myth 3: Sun Exposure Has No Impact on Dermatomyositis
Fact:
Exposure to UV rays can trigger, worsen, or flare rashes in DM patients.
Sunlight increases inflammation in already sensitive skin and activates immune pathways. Even indoor lighting sources (like halogen lamps) can worsen rashes in rare cases.
Dermatologists strongly advise:
- Using sunscreen SPF 50+
- Wearing full sleeves and hats
- Avoiding peak sunlight hours
- Using UV-protective window films
- Choosing mineral sunscreens (zinc oxide, titanium dioxide)
Sun protection is not optional—it is a core part of DM treatment.
Myth 4: Exercise Makes Muscle Weakness Worse
Fact:
Safe, supervised exercise improves DM-related muscle weakness.
Historically, patients were advised to avoid physical activity. But modern research shows that controlled exercise reduces inflammation, improves strength, and enhances overall ability.
Beneficial exercises include:
- Low-impact aerobic workouts
- Physical therapy–guided muscle training
- Stretching routines
- Yoga modified for autoimmune patients
Patients should avoid overexertion during flare-ups but completely avoiding exercise worsens disability.
Myth 5: Steroids Alone Can Cure Dermatomyositis
Fact:
Steroids control inflammation but cannot cure DM.
Dermatomyositis requires long-term management, often including:
- Corticosteroids
- Immunosuppressants (azathioprine, methotrexate, mycophenolate)
- Biologic agents (rituximab)
- IVIG therapy
- Physical therapy
- Sunscreen and skin care
Steroids help quickly reduce inflammation but are not a permanent solution. Uncontrolled steroid use can also cause serious side effects.
Long-term remission requires a multidisciplinary treatment approach.
Myth 6: Dermatomyositis Always Indicates Cancer
Fact:
DM is associated with a higher cancer risk—but it does not mean everyone has or will develop cancer.
About 15–20% of adults with DM may have underlying malignancy, but the majority do not.
Common associated cancers include:
- Ovarian
- Lung
- Breast
- Colon
- Lymphoma
Doctors recommend appropriate cancer screening at diagnosis and periodically afterward.
This is precautionary, not because every patient will develop cancer.
Myth 7: Dermatomyositis Is Always Progressive and Untreatable
Fact:
Many patients achieve long-term remission with proper treatment.
With early diagnosis and appropriate therapy, patients can:
- Regain muscle strength
- Reduce skin rashes
- Prevent lung involvement
- Lead active, productive lives
DM severity varies from person to person. Some experience mild symptoms, while others may have aggressive disease—but treatment works in most cases.
Myth 8: Dermatomyositis Is Contagious
Fact:
DM is not contagious, infectious, or spread through contact.
It is an autoimmune condition caused by an abnormal immune response—not bacteria or viruses. No one can “catch” dermatomyositis from another person.
Myth 9: Symptoms Are Only Physical—Mental Health Is Not Affected
Fact:
Autoimmune diseases significantly affect mental and emotional well-being.
Common issues include:
- Anxiety
- Depression
- Body image concerns due to skin changes
- Social withdrawal
- Fatigue-related mood problems
Supportive counseling, stress management, and patient support groups can greatly improve quality of life.
How to Manage Dermatomyositis Effectively: Patient Tips
Here are simple but powerful steps:
✔ Take medicines regularly
Skipping doses increases flare risk.
✔ Protect skin from sunlight
Broad-spectrum sunscreen, protective clothing, and shade are essential.
✔ Follow a tailored exercise program
Strength training + stretching + physiotherapy = better recovery.
✔ Eat an anti-inflammatory diet
Include omega-3s, leafy greens, turmeric, berries, whole grains.
✔ Track symptoms
Note fatigue, rashes, breathing issues, weakness progression.
✔ See specialists regularly
Rheumatologist + dermatologist + pulmonologist depending on symptoms.
Conclusion
Dermatomyositis is a complex autoimmune disease, but most myths surrounding it are not true. Understanding the actual facts helps in:
- Early diagnosis
- Better treatment outcomes
- Reduced anxiety
- Improved daily life and long-term prognosis
With proper nutrition, sun protection, exercise, medication, and regular follow-up, patients can manage the disease effectively and lead a fulfilling life.
FAQs on Dermatomyositis: Myths, Risks & Management
1. Is dermatomyositis curable?
There is no permanent cure yet, but many patients achieve partial or full remission with early and consistent treatment.
2. Is dermatomyositis genetic?
Not directly. Genetics may increase susceptibility, but DM is not inherited.
3. How long does it take for symptoms to improve?
Many patients notice improvement within 6–12 weeks, but full recovery may take months to years depending on severity.
5. Does stress worsen dermatomyositis?
Yes. Stress can trigger immune system activation and flare-ups.
6. Can children fully recover from juvenile dermatomyositis?
Many children achieve excellent long-term outcomes with timely treatment.
7. Are rashes permanent?
Rashes improve with treatment but may recur with sun exposure or disease flare.