Living with Psoriatic Arthritis (PsA) can be challenging, but nighttime flare-ups—when pain, stiffness, and discomfort suddenly worsen—are among the most frustrating. Many people find that their joints feel fine or manageable during the day, but the moment they lie down to sleep, the pain intensifies. This can lead to disturbed sleep, daytime fatigue, anxiety, and even higher disease activity.
If you’ve ever wondered “Why does my Psoriatic Arthritis hurt more at night?”, this comprehensive guide will help you understand the science behind nighttime flares and provide practical, proven sleep solutions.
What Are Nighttime Flares in Psoriatic Arthritis?
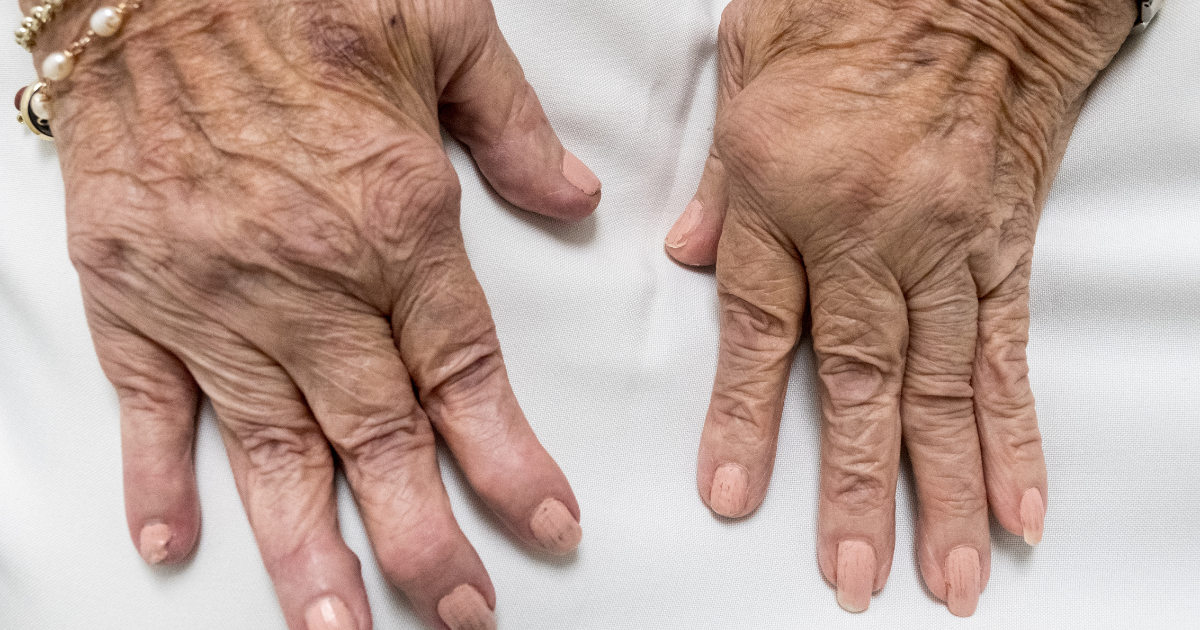
A nighttime flare means your Psoriatic Arthritis symptoms—pain, stiffness, swelling, tingling, or burning—worsen significantly during the late evening or while you sleep. It often affects:
- Finger and toe joints
- Wrists and elbows
- Knees and ankles
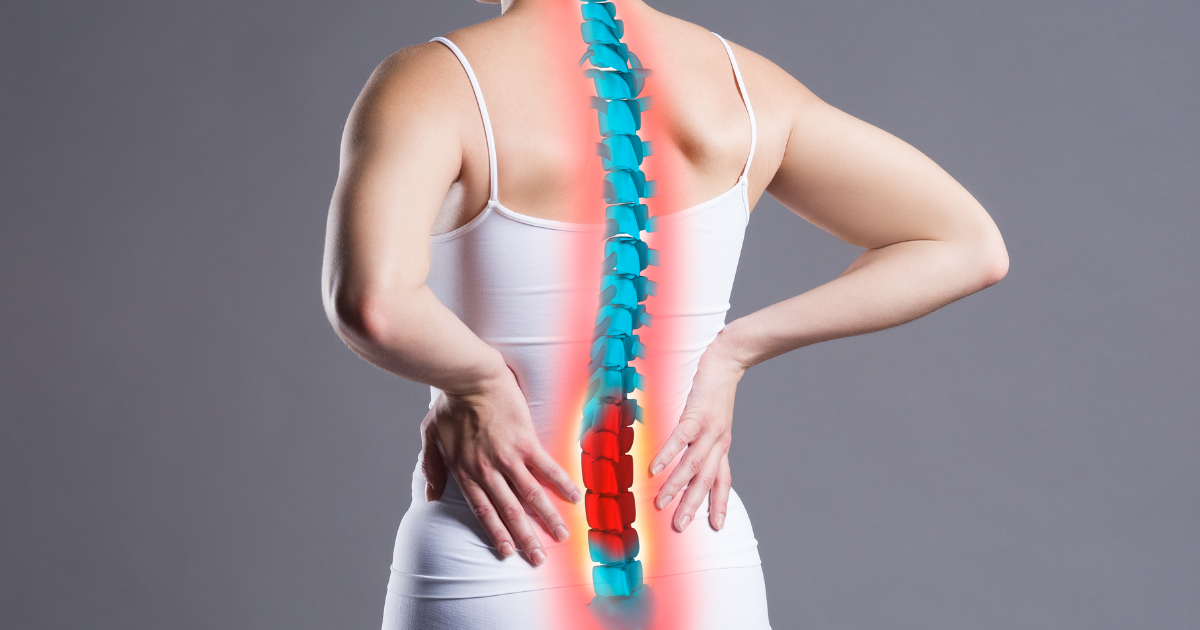
- Lower back (common in axial PsA)
- Tendons (Achilles, plantar fascia, etc.)
These nighttime issues are not imagined—they are real and have biological reasons behind them.
Why Psoriatic Arthritis Flares at Night: The 8 Most Common Causes
Below are the scientifically supported reasons PsA pain tends to worsen at night.
1. Natural Circadian Rhythm Increases Inflammation at Night
Your body follows a 24-hour biological clock, called the circadian rhythm. This rhythm affects hormone levels, immunity, and inflammation.
At night:
- Anti-inflammatory hormones such as cortisol naturally drop
- Pro-inflammatory cytokines such as IL-6, TNF-α, and IL-17 rise
This creates a perfect environment for PsA-related inflammation to spike.
Result: More stiffness, deep joint pain, and throbbing while trying to sleep.
2. Reduced Movement Leads to Joint Stiffness
During the day, your joints stay lubricated because you move frequently. At night:
- You lie still for long hours
- Joint fluid circulation decreases
- Muscles stiffen
- Tendons tighten
When the joints stay inactive too long, inflammation accumulates, making PsA pain worse.
3. Temperature Drop at Night Triggers Pain
Body temperature decreases slightly during sleep. For people with PsA, this can cause:
- Muscle tightening
- Increased joint stiffness
- Slow blood flow to extremities
- Heightened nerve sensitivity
Cold bedrooms or winter months often worsen nighttime pain.
4. Stress Accumulates by Nighttime
The stress hormone cortisol is naturally lowest at night, but mental stress from the day still affects the body. Stress increases inflammatory cytokines, potentially triggering:
- Tendon pain
- Joint swelling
- Skin flare-ups
Many patients report nighttime flares after emotionally tiring days.
5. Poor Sleep Position Overloads Joints
Sleeping in certain positions can put direct pressure on joints affected by PsA.
Common examples:
- Side sleeping → hip, shoulder, and knee pain
- Stomach sleeping → lower back and neck strain
- Wrong pillow height → spinal misalignment
Pressure on already inflamed joints worsens nighttime discomfort.
6. Obesity or Sudden Weight Change
Higher body weight adds mechanical load to joints. At night, inflammation concentrates in:
- Knees
- Ankles
- Hips
- Lower back
Fat cells also produce inflammatory chemicals (adipokines), which intensify PsA symptoms.
7. Untreated Sleep Disorders
Sleep problems are extremely common in Psoriatic Arthritis and may worsen nighttime flares:
- Sleep apnea (breathing stops repeatedly during sleep)
- Restless legs syndrome
- Insomnia caused by anxiety or depression
These conditions increase systemic inflammation, making Psoriatic Arthritis pain worse.
8. Medication Timing May Not Cover Nighttime Pain
If your Psoriatic Arthritis medications—NSAIDs, DMARDs, biologics, or steroids—peak during the day, their effect may wear off by bedtime.
This can leave a “pain gap” at night.
Symptoms That Indicate Nighttime PsA Flares
Common symptoms include:
- Increased joint stiffness when lying down
- Throbbing or pulsating pain in hands or feet
- Burning sensation in joints
- Lower back pain worse at night (axial PsA)
- Swollen hands or toes (sausage digits)
- Difficulty turning sides
- Cramping in feet or calves
- Tingling or numbness
If these symptoms frequently interrupt sleep, your PsA is likely active and needs attention.
How Nighttime PsA Flares Affect Your Health
Poor sleep has long-term consequences:
1. Increased Daytime Pain Sensitivity
Your brain becomes more sensitive to pain when sleep is poor.
2. Higher Levels of Inflammation
Lack of sleep raises inflammatory markers, which worsen PsA progression.
3. Mood Changes
Nighttime pain increases:
- Anxiety
- Irritability
- Fatigue
- Depression
4. Lower Immunity
Poor sleep weakens immunity, potentially making skin psoriasis worse.
Practical Sleep Solutions for Nighttime PsA Flares
1. Adjust Your Sleep Position (The Right Way)
Best position:
Back sleeping with a pillow under knees
→ reduces pressure on spine, hips, and knees.
If you sleep on your side:
- Place a pillow between knees
- Keep spine straight
- Avoid curling too tightly
Avoid:
- Stomach sleeping
- Very thick pillows
- Collapsed old mattresses
2. Use Heat Therapy Before Bed
Heat helps relax muscles, improve blood flow, and reduce stiffness.
Options:
- Warm shower before bed
- Heating pad on joints (10–15 minutes)
- Warm water foot soak
- Electric blanket on low
If joints are swollen, use cold packs for 5–7 minutes first.
3. Maintain a Warm Sleep Environment
Try to keep bedroom temperature between 22–24°C (71–75°F).
Tips:
- Wear warm socks
- Use layered blankets
- Avoid sleeping in direct AC or fan airflow
Cold triggers joint and tendon flare-ups in PsA.
4. Improve Sleep Hygiene
Consistent sleep routine reduces inflammation.
- Sleep and wake at the same time daily
- Avoid heavy phone use before bed
- Use dim lights after 9 pm
- Avoid caffeine after 4 pm
- Use your bed only for sleep
5. Light Stretches Before Bed
Gentle stretching for 5–8 minutes can significantly reduce nighttime stiffness.
Focus on:
- Lower back
- Hips
- Hamstrings
- Ankles
- Shoulders
Yoga poses like child’s pose, cat-cow, or gentle hip openers help.
6. Anti-inflammatory Nighttime Snack
Eat 1 hour before bed:
- Warm turmeric milk
- Almonds or walnuts
- Kiwi (improves sleep)
- Cherries (natural melatonin)
Avoid heavy dinner, sugar, or junk foods.
8. Manage Stress and Anxiety
Try:
- Deep breathing
- Mindfulness apps
- Gratitude journaling
- Relaxation audio
- Progressive muscle relaxation
Reducing stress lowers nighttime inflammatory surges.
9. Treat Underlying Sleep Disorders
If you snore, gasp, or feel extremely tired during the day, you may have sleep apnea.
Treating sleep disorders dramatically reduces PsA pain.
When to See Your Rheumatologist
Seek medical advice if:
- Nighttime pain wakes you regularly
- Morning stiffness lasts >45 minutes
- Swelling increases suddenly
- You feel extremely fatigued
- Your sleep is affected for more than 2 weeks
- Over-the-counter painkillers do not help
Persistent nighttime flares indicate active Psoriatic Arthritis, and early adjustments in treatment can prevent long-term joint damage.
Conclusion
Nighttime Psoriatic Arthritis flares are extremely common and rooted in real biological mechanisms like circadian rhythm changes, inactivity during sleep, cold temperatures, stress, and joint overload.
The good news:
With the right sleep habits, joint protection strategies, heat therapy, and optimized medication timing, you can significantly reduce nighttime pain and finally get restful sleep.