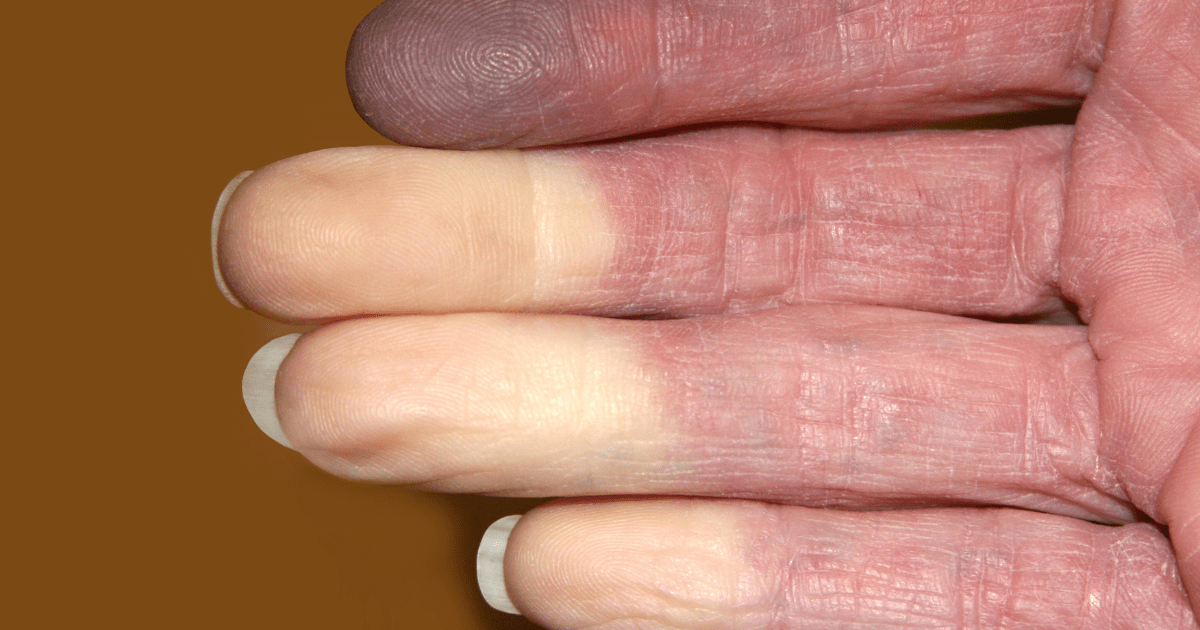
Your fingers turn white, then blue, then red. They go numb, sting, or throb. These color shifts might seem harmless, but in the context of scleroderma, they could be the start of something more serious.
This phenomenon—known as Raynaud’s—is not just a reaction to cold. In scleroderma, it reflects blood vessel damage that can lead to painful ulcers, infection, and tissue loss if ignored.
Let’s understand how these color changes evolve into complications, and what you can do to prevent them.
What Is Raynaud’s Phenomenon?
Raynaud’s is a vascular condition where small blood vessels temporarily constrict, limiting blood flow—usually in the fingers or toes. It’s triggered by cold or stress.
In scleroderma, this is called secondary Raynaud’s, and it’s often more severe and progressive than the primary type.
The Three-Stage Color Changes in Raynaud’s
Each Raynaud’s episode typically follows a three-color pattern, indicating different phases of blood flow restriction:
1️⃣ White (Ischemia)
Blood flow is significantly reduced due to vessel spasm. Fingers feel cold and numb.
2️⃣ Blue (Cyanosis)
Oxygen levels drop. Tissues turn bluish-purple. There may be tingling or burning sensations.
3️⃣ Red (Reperfusion)
Blood returns suddenly, causing redness, throbbing, or swelling. This phase can be painful.
Duration of an episode can range from minutes to over an hour, depending on the trigger and severity.
Why Raynaud’s Is Worse in Scleroderma
In scleroderma, the small blood vessels are not just constricting—they are also damaged and inflamed. Over time, this leads to:
- Thickening of vessel walls
- Reduced blood flow permanently
- Poor oxygen supply to fingers and toes
This chronic issue sets the stage for serious complications.
Complications of Raynaud’s in Scleroderma
While the initial symptoms may seem manageable, Raynaud’s in scleroderma can result in:
🔸 Digital Ulcers
Painful sores on fingertips due to poor blood supply. Slow to heal and prone to infection.
🔸 Calcinosis
Calcium deposits under the skin, which may break through and become painful.
🔸 Skin Atrophy & Scarring
Chronic lack of oxygen leads to thinning skin and permanent damage.
🔸 Gangrene & Tissue Loss
In extreme cases, untreated ulcers may result in gangrene, requiring amputation.
Prevention and Management
Lifestyle Changes
- Dress warmly: Use thermal gloves and socks in cold weather
- Avoid triggers: Sudden cold, emotional stress, caffeine, and nicotine
- Moisturize daily: Keeps skin soft and reduces ulcer risk
Medical Treatment
- Vasodilators: Nifedipine or amlodipine to improve blood flow
- Topical nitrates: For local circulation
- Immunosuppressants: For underlying scleroderma
- Advanced therapies: Botox, prostacyclin infusions, or sympathectomy for severe cases
When to See a Doctor?
If you notice:
- Frequent color changes even without cold exposure
- Painful or infected ulcers
- Cracking or open sores on fingers
- Any signs of dry gangrene or blackened skin
See a rheumatologist immediately. Early intervention can prevent long-term damage.
FAQs: Raynaud’s in Scleroderma
Q1. Does every person with scleroderma get Raynaud’s?
Almost 90% of scleroderma patients experience Raynaud’s as an early symptom.
Q2. Are the color changes dangerous?
The color changes themselves aren’t dangerous—but they signal underlying vascular problems that can lead to serious damage if ignored.
Q3. Can ulcers from Raynaud’s heal on their own?
Sometimes minor ones may, but most require treatment to avoid infection or complications.
Q4. Can stress alone trigger Raynaud’s?
Yes. Emotional stress, like cold, causes vessel constriction and can trigger an attack.
Q5. Is Raynaud’s curable?
There’s no cure, but it can be well managed with lifestyle changes and medications.
Final Thoughts
Raynaud’s might seem like just a color-changing quirk of your body—but for people with scleroderma, it’s a warning bell. These episodes mark the beginning of a vascular journey that could lead to painful complications without proper care.
Don’t wait for ulcers or pain to take action. If you or a loved one experience these symptoms, consult a specialist early and take proactive steps to protect your hands, your skin, and your quality of life.